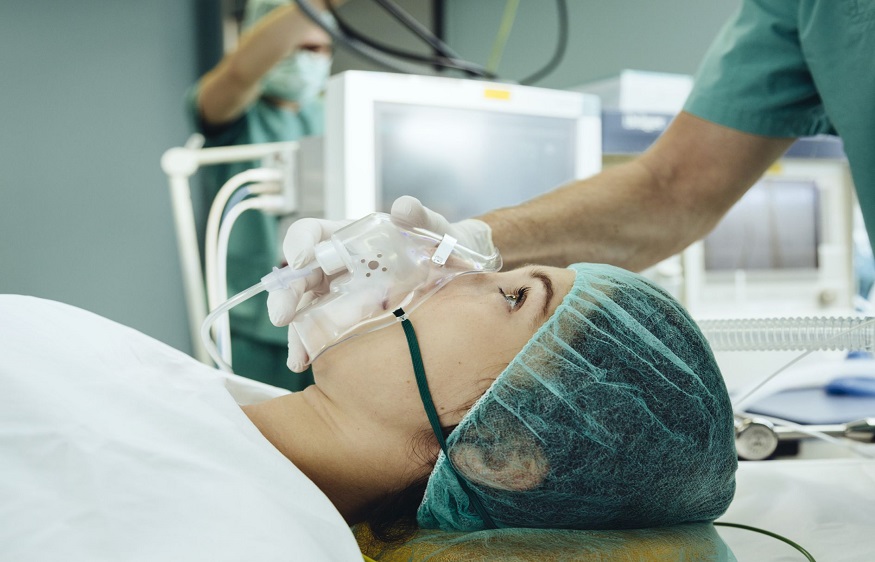
What Is General Anaesthesia And Its Adverse Effects? When And How Is It performed?
General anaesthesia is a type of anaesthesia by which the patient is entirely asleep so that they do not feel any pain or be aware during the performance of a specific intervention. The patient will not remember what has happened to him during the period that he has been asleep.
What is general anaesthesia?
General anaesthesia numbs and relaxes the entire body, suppressing some of the functions that our body performs automatically. This numbness includes the nerves that control breathing, blood pressure, heart rate, the ability to swallow (swallow), etc. For all these reasons, it is required that a doctor, called an anesthesiologist, be present during general anaesthesia, who is in charge of gradually administering the anaesthetic and monitoring that all these bodily functions continue to function correctly.
When is general anaesthesia performed?
Most major surgeries are performed under general anaesthesia. Most surgical interventions and uncomfortable diagnostic tests in children are also served with this anaesthesia since it allows the child to be asleep and not feel anything during the procedure.
How should the patient prepare for general anaesthesia?
Before anaesthesia, the patient must have a pre-anaesthetic consultation with the anaesthesia specialist. During this visit, the patient must tell the doctor all the diseases, allergies and medications that he is taking. Some medicines can interfere with the anaesthesia that will be given, reducing or increasing its effects. It would help if you also discussed the possibility of a pregnancy.
The anesthesiologist will inform the patient which medications she must abandon and how far in advance.
The anaesthetist usually orders a blood test and sometimes an EKG and chest X-ray.
Before general anaesthesia, the anaesthetist should explain the risks associated with anaesthesia for that particular person.
Contraindications of general anaesthesia
In general, there are no absolute contraindications to performing general anaesthesia. However, in certain circumstances, the risk of complications during anaesthesia is more significant, generally circumstances related to previous illnesses or problems of the patient. In these situations, the risk of the operation must be properly assessed against the benefits obtained with it and act accordingly.
How is general anaesthesia performed?
The patient attends fasting for anaesthesia. Going on an empty stomach is essential because this prevents liquid or food from being in the stomach, which could pass into the lungs during anaesthesia and cause various complications.
When a patient is going to be anaesthetised, they are already in the operating room, and a peripheral line has been placed (a vein has been cannulated). Wires have also been placed on his chest to monitor the electrical activity of his heart continuously, a cuff on his arm to monitor blood pressure, and a clamp (saturometer) has been placed on his finger, which measures the oxygenation of the blood.
Anaesthesia can be induced by injecting medication into a vein, inhaling a gas through a mask, or both.
Subsequently, the patient is intubated (a tube is inserted into the trachea) and artificially ventilated through said tube (pressurized air is introduced to help the patient breathe) since anaesthesia paralyzes the muscles of the trachea Breath. The air introduced through the tracheal tube contains a certain amount of oxygen and anaesthetic gas that keeps the patient asleep. The anaesthetic, in addition to the gas, can continue to be introduced through the vein.
The anesthesiologist will be aware of the patient’s blood pressure, heart rate, oxygenation and other circumstances so that there are no complications.
When the patient is anaesthetized, he will not notice anything and will not remember anything that has happened to him.
Adverse effects of general anaesthesia
General anaesthesia can have, although infrequently, adverse effects, some fatal. In general, the negative impact of this anaesthesia is more excellent than those found with local anaesthesia or regional anaesthesia. Adverse effects are usually few in healthy people but can be more significant if underlying diseases exist. The most frequent or severe are:
- Allergies to anaesthesia.
- Longer than the usual effect of anaesthesia.
- Injuries to the teeth, tongue, larynx or trachea result from the tube inserted into the trachea.
- Aspiration of contents of the mouth or digestive system into the lungs. Since there are no reflexes such as swallowing, coughing, or throat clearing during anaesthesia, any fluid that passes into the lungs cannot be expelled, leading to complications such as aspiration pneumonia. In general, it is an infrequent complication since the tube inserted into the trachea also blocks the passage of any content towards the lungs.
- Nausea and vomiting. They occur more frequently after abdominal operations.
- Changes in heart rate or blood pressure.
- Arrhythmias.
- Stroke.
- Myocardial infarction.
- Temporary mental confusion (delirium).
- Death.
Is there any aftercare necessary after general anaesthesia?
After general anaesthesia, the patient must wake up in an area of the hospital called resuscitation.
The patient wakes up dizzy and confused. This subsequent numbness has a variable duration depending on the type of anaesthetic used, its dose and the patient’s characteristics.
There may also be nausea, vomiting, chills and cramps.
Sometimes there is discomfort in the throat due to the introduction of the tracheostomy tube. This discomfort may barely exist or may last for several days. Sometimes such pain is accompanied by hoarseness due to damage to the larynx



Average Rating